A patient once said, “The injection helped for a few days, but then the pain came back — and I felt like I was right back where I started.”
That experience is more common than many people realize.

Steroid injections have been used for years to reduce inflammation and calm pain in joints, tendons, and surrounding tissues. In the right situation, they can be useful. They may help settle down a painful flare, reduce irritation in bursitis, or provide short-term relief when symptoms are limiting daily function. Current guidance still supports corticosteroid injections as one option for short-term symptom relief in selected musculoskeletal conditions.
But short-term relief and long-term recovery are not the same thing.
At Innerve8 Medical, we believe the more important question is not just, “How do we calm the pain?” It is, “Why is this tissue irritated in the first place?”
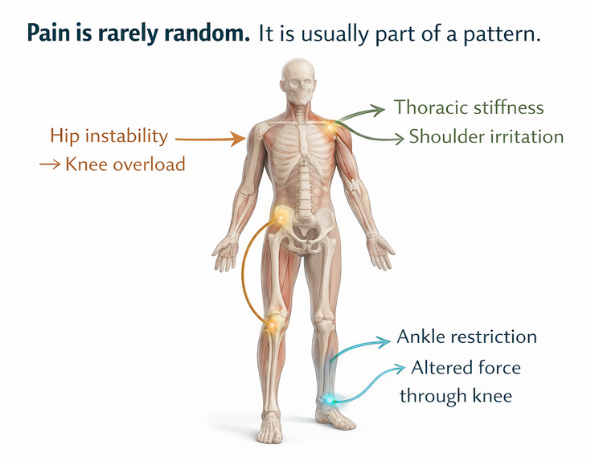
Because pain is rarely random. It is usually part of a pattern.
A knee may be taking more force than it should because the hip is not controlling movement well. A shoulder may keep becoming inflamed because the upper back is stiff and the scapula is not moving efficiently. A tendon may stay irritated not because it is “bad,” but because it is repeatedly being asked to handle more load than the body can currently manage.
That is where many treatment conversations need to go deeper.
What steroid injections actually do
Corticosteroid injections are designed to reduce inflammation. That can make them helpful when inflammation is a major driver of symptoms. Many patients feel relief quickly, which is one reason these injections remain common. They can absolutely have a place when used thoughtfully, selectively, and with a clear clinical reason.
The limitation is that they do not automatically fix the reason the area became overloaded.
If movement quality is poor, if joint mechanics are off, if tissue capacity is low, or if the same compensation pattern keeps repeating, pain relief alone may not solve the bigger problem. It may simply quiet symptoms for a period of time while the underlying stress remains.
That is often why pain returns.
Where caution matters
Steroid injections are not risk-free. Reviews and current recommendations describe local risks such as skin thinning or color change at the injection site, infection, tendon injury, and concern for cartilage-related damage in some settings. Systemic effects such as temporary blood sugar elevation and adrenal suppression can also occur, which is especially relevant for patients with diabetes or other medical considerations.
That does not mean steroid injections are always the wrong choice. It means they should be used with intention.
The concern becomes greater when injections are repeated without stepping back and reassessing the situation. Current guidance emphasizes timing, spacing, and shared decision-making rather than reflexively repeating injections every time symptoms flare up.
In other words, a steroid injection may help in the short term, but it should not become the automatic answer every time pain returns.
The bigger issue: what is driving the overload?
This is where Innerve8 Medical takes a different approach.
We do not look only at the painful area. We look at how the body is functioning as a system. That includes joint motion, posture, range of motion, movement quality, compensation patterns, tissue loading, and the relationship between one area and another.
For example, recurring knee pain may involve hip control, ankle restriction, or poor load transfer. Shoulder pain may reflect thoracic stiffness, scapular mechanics, or repetitive overload. Tendon pain may come from a mismatch between activity demands and the tissue’s current capacity to recover.
That kind of evaluation matters, because treatment should match the reason the problem keeps happening.
Where regenerative therapies may fit
For some patients, especially those with recurring pain, tendon irritation, or degenerative joint issues, regenerative therapies may be worth discussing as part of a broader non-surgical plan.
Platelet-Rich Plasma, or PRP, is one of the best-known options. Unlike steroids, which are intended to suppress inflammation, PRP is designed to support the body’s own repair signaling using a concentrated portion of the patient’s own blood. Evidence for PRP is encouraging in some conditions, particularly knee osteoarthritis, where recent reviews have found better pain and functional outcomes than corticosteroid injections over longer follow-up in some patient groups. At the same time, the research is still mixed in some areas, and outcomes can vary based on diagnosis, protocol, and patient selection.
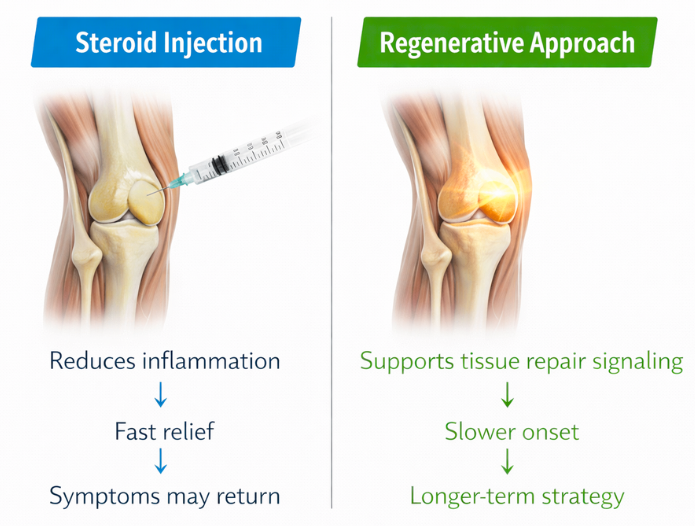
That nuance matters.
PRP is not a universal solution. It is not right for every patient, and it usually works more gradually than a steroid injection. But for the right patient, it may offer a more biologically constructive option than repeatedly suppressing symptoms without addressing the underlying issue.
A better question to ask
The smartest question is usually not, “Which injection works fastest?”
It is, “What is the real goal of treatment, and what problem are we actually trying to solve?”
If someone is dealing with a severe inflammatory flare, a steroid injection may still make sense. But if pain keeps returning, function is declining, or the same area repeatedly breaks down under normal activity, it may be time to stop chasing temporary relief and look deeper.
At Innerve8 Medical, that is where we start.
We believe in evaluation before treatment. We believe in understanding structure, movement, tissue stress, and recovery before deciding what comes next. And we believe that for many patients, the real opportunity is not just to quiet pain for a few days or weeks, but to understand why the body keeps asking for help in the first place.
If this sounds familiar, call (703) 739-0500 or schedule an evaluation here. This is something we assess every day, and for the right patient, a more complete strategy may make more sense than repeating the same cycle.


