For many people, migraines are more than “just headaches.” They’re disruptive, exhausting, and often unpredictable.
Patients do what they’re told — take prescribed medications, try Botox, manage stress, adjust lifestyle habits — yet the migraines keep coming. Over time, the pain may begin to feel more complex: pressure at the temples, tightness in the jaw, stiffness in the neck, or pain at the base of the skull.
For some patients, this isn’t random.
It’s a pattern.
Migraines are neurological — but their triggers aren’t always in the head
Migraines involve abnormal pain signaling in the nervous system. But where those signals are triggered — and what keeps them active — can vary from person to person.
In many cases, the source of ongoing irritation lies outside the head itself, in areas that are often overlooked during traditional migraine care. One of the most commonly missed contributors is the jaw joint.
What is TMJ — and why does it matter?
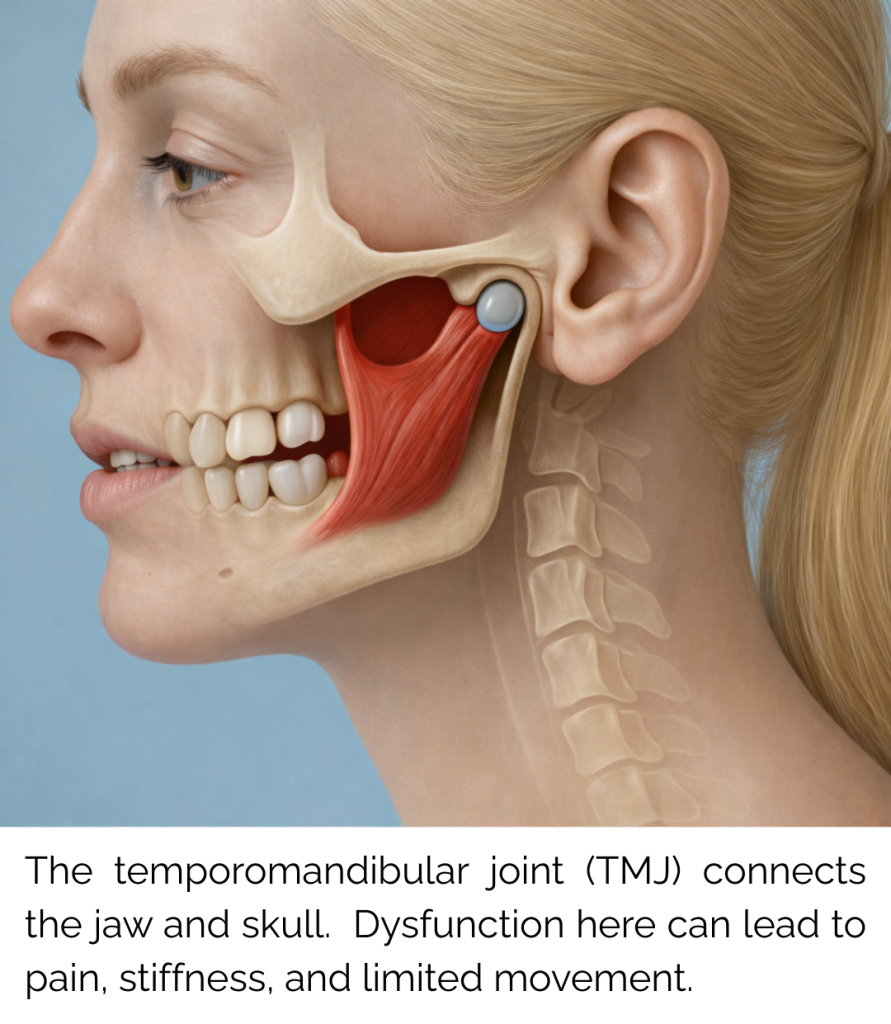
TMJ refers to the temporomandibular joint, which connects the jaw to the skull. It’s used constantly — talking, chewing, clenching, yawning, even during sleep.
The jaw joint and surrounding muscles sit extremely close to key nerves that supply sensation to the face, temples, and back of the head — including pathways commonly involved in migraines.
When the TMJ or nearby muscles become irritated, overworked, or dysfunctional, pain doesn’t always stay in the jaw. It can travel upward, presenting as temple pain, facial pressure, neck tightness, or migraine symptoms that feel difficult to explain.
The pattern many patients don’t realize is connected
Patients with TMJ involvement often describe a familiar combination of symptoms:
- Deep or pressure-like pain in the temples
- Jaw tightness or clenching, especially during stress or sleep
- Neck and upper back tension
- Tenderness at the base of the skull
- Migraines that persist despite medication or injections
When these symptoms appear together, it’s often not a coincidence.
It’s a pattern — and patterns matter when it comes to chronic pain.
Why this connection is often missed
Migraine care is frequently siloed. Neurology focuses on the brain. Dentistry focuses on the bite. Orthopedics focuses on joints. Each discipline plays an important role, but chronic pain rarely belongs to just one system.
TMJ dysfunction and myofascial pain don’t always show up clearly on imaging. Many patients are told scans look “normal,” even while symptoms continue. Over time, the nervous system can become sensitized, allowing pain signals to remain active long after the original trigger has been overlooked.
A systems-based approach to migraines
At Innerve8 Medical, we take a broader view. We evaluate how the jaw, cervical spine, muscles, and nerves work together — because lasting relief often depends on addressing more than one contributor.

For the right patient, treatment may focus on calming irritated nerve pathways, releasing overactive muscle trigger points, and supporting the jaw joint itself. This can include targeted therapies to deactivate painful muscle knots, nerve-focused treatments to reduce sensitization at the base of the skull, and joint-specific interventions designed to reduce inflammation and restore healthier movement patterns.
The goal isn’t to chase symptoms.
It’s to understand what’s driving them.
Who this information may be relevant for
This approach may be worth exploring if you:
- Experience migraines along with jaw or neck pain
- Notice jaw tightness or clenching during stress or sleep
- Feel pain at the temples or base of the skull
- Have tried multiple migraine treatments with limited success
Migraines don’t have a single cause — and they shouldn’t be approached with a one-size-fits-all solution.
The first step is clarity
Understanding how your symptoms fit together can change the trajectory of care. For some patients, identifying and addressing TMJ involvement is the missing piece that allows the nervous system to settle and pain patterns to improve.
If this sounds familiar, a comprehensive evaluation can help clarify what’s contributing to your migraines and whether a systems-based approach may be appropriate.
Book an appointment at www.innerve8medical.com or call (703) 739-0500. Clarity is often the first step toward lasting relief.


